Diabetic Eye Disease
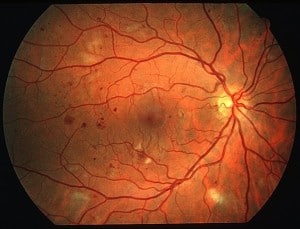
Over 40 percent of patients diagnosed with diabetes develop some form of eye disease as a result of their Diabetes. Diabetic Retinopathy is the most common diabetic eye disease and a primary cause of blindness in the United States.
Diabetes can damage blood vessels in the eye, causing blood or fluid to leak into the retina, the light-sensitive tissue at the back of the eye. It can also cause new blood vessels to grow on the surface of the retina, leading to significant damage to vision and the overall quality of life.
Diabetic eye disease is a combination of various eye conditions that develop as a result of diabetes. These conditions include:
- Diabetic Retinopathy
- Cataracts
- Glaucoma
- Dry Eye
Stages of Diabetic Retinopathy
There are four distinct stages of diabetic retinopathy:
- Mild nonproliferative retinopathy – microaneurysms develop in the tiny blood vessels of the retina
- Moderate nonproliferative retinopathy – blood vessels to the retina start to leak and even bleed
- Severe nonproliferative retinopathy – the blood supply to the retina is blocked
- Proliferative retinopathy – New blood vessels appear in the retina as a response to blocked blood flow. These “new vessels” are very fragile and easily hemorrhage.
During any stage of diabetic retinopathy a condition known as macular edema can develop. Macular edema is the buildup of fluid in the macula, the light-sensing part of the retina that allows us to see objects with great detail. As the macula swells vision becomes blurred. About half of the people with proliferative retinopathy are diagnosed with macular edema.
Symptoms of Diabetic Retinopathy
Early stages of Diabetic Retinopathy usually do not show symptoms. Treatment is not always required. Patients need to monitor their blood sugar level to prevent the disease from progressing. If the disease does progress, prompt treatment will be necessary to preserve your vision.
Symptoms of Diabetic Retinopathy may include the following:
- Vision that may be blurry or doubled
- Blind spots
- Dark floaters or spots in the vision
- Problems with peripheral vision
- Severe vision loss or blindness
Diagnosis of Diabetic Retinopathy
After a thorough medical examination of the eyes, some of the following diagnostic tests will be conducted to confirm diagnosis:
- Visual acuity test
- Dilated eye examination
- Tonometry test
- Retinal exam
- Fluorescein angiogram
- Optical Coherence Tomography (OCT)
Treatment of Diabetic Retinopathy
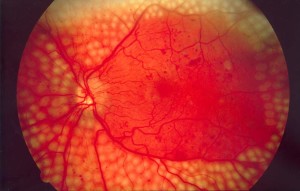
Treatment for macular edema sometimes includes a laser procedure called focal laser treatment. During this procedure, several hundred small laser burns are placed in the areas of retinal leakage around the macula to prevent leakage from occurring and reduce the amount of fluid in the retina. This helps reduce the risk of vision loss and may improve lost vision in a small number of cases. Focal laser treatment is performed in your doctor’s office and can usually be completed in just one session.
Reducing the Risks of Developing Diabetic Retinopathy
Patients with diabetes need to have an annual comprehensive dilated eye exam. The length of time a patient has diabetes will determine the likelihood of developing diabetic retinopathy. Over 40 percent of patients in the United States, diagnosed with diabetes, have a form of diabetic retinopathy.
The risks of developing diabetic eye disease can be minimized by:
- Monitoring changes in vision
- Keeping A1C levels under 7%
- Monitoring and managing blood pressure levels
- Eating a healthy diet
- Participating in a regular exercise routine
- Monitoring and managing cholesterol levels
